Two-stage orthodontic treatment outcomes of children with dentoalveolar class II malocclusion
- Authors: Ayupova F.S1, Khotko R.A1
-
Affiliations:
- Kuban State Medical University
- Issue: Vol 103, No 1 (2022)
- Pages: 133-142
- Section: Clinical observations
- Submitted: 21.05.2021
- Accepted: 24.11.2021
- Published: 07.02.2022
- URL: https://kazanmedjournal.ru/kazanmedj/article/view/70895
- DOI: https://doi.org/10.17816/KMJ2022-133
- ID: 70895
Cite item
Abstract
Background. During the rehabilitation of children with distal occlusion, it is not always possible to achieve the desired outcomes. In this context, the factors influencing the outcomes of treatment for class II malocclusions in children at different stages of occlusion development.
Aim. To study two-stage orthodontic treatment outcomes in children with dentoalveolar class II malocclusion by the clinical case.
Material and methods. We analyzed the physical examination results of the patient within the treatment from 6 to 17 years. Facial proportion symmetry, aesthetic, type of face, plaster dental models were determined by using the photographs. Orthopantomography was used to analyze the condition of temporary and permanent teeth, jaw bone tissue and to assess functional disorders. Orthodontic treatment in a mixed dentition period was carried out using removable devices, including those improved by the authors. In the permanent dentition, orthodontic brackets with power elements were used.
Results. Untimely contacting the doctor, an insufficient level of motivation to implement recommendations for improving posture and dental care contributed to an increase in treatment duration. Keeping excessive cervical spine flexion and head tilted back, the “bad habit” of placing (pressure) the hand on the chin, and the rejection of a myo-gymnastic exercise (physical therapy) interfered with the synchronous (normal) development of the jaws. Premature loss of a temporary molar on one side led to dentoalveolar asymmetry and disruption of occlusal contacts. Additional orthodontic appliances were used to correct these deformities. Over-retained deciduous teeth led to the delayed eruption of permanent teeth and, presumably, to the curvature of their roots. Violation of the tooth’s root shape and asymmetry in permanent teeth crown size prevented the full correction of their position using highly effective modern non-removable orthodontic equipment. The anomalous position of the rudiment of the third molar, the refusal for timely tooth extraction further led to the increasing complexity of the surgical technique.
Conclusion. The timing and effectiveness of orthodontic treatment of a patient with dentoalveolar class II malocclusion were influenced by a poor body posture, extraction of a primary molar, the delayed eruption and crown size asymmetry of permanent teeth, the presence of “bad” habits and minimal cooperation of the patient with the orthodontist.
Keywords
Full Text
Актуальность
Дистальная окклюзия (ДО) — распространённая патология, которую выявляют не менее чем у 11% детей при профилактическом осмотре и более чем у 40% детей, обратившихся за ортодонтическим лечением, в том числе у детей Краснодарского края [1–5].
ДО в периоде постоянного прикуса нередко сочетается с аномалиями формы и размеров зубных дуг, тесным положением зубов, аномалиями положения резцов, вестибулопозицией клыков, что вызывает у пациента эстетический дискомфорт, приводит к ухудшению гигиены полости рта и влияет на качество жизни пациентов [1, 2, 6–9].
Комплексная реабилитация детей с ДО направлена на достижение гармоничности лица, нормализацию положения зубов, формы и размеров зубных рядов и их соотношения, функционального состояния жевательных и мимических мышц [1, 2, 7, 10–13].
Ортодонтическое лечение, начатое при первых признаках формирующейся ДО, сопровождается продолжительным применением съёмных и несъёмных ортодонтических устройств, перестройкой состояния жевательных и мимических мышц, нормализацией функций дыхания, жевания, глотания, речи [1, 2, 6, 9–21].
В ходе реабилитации детей с ДО не всегда удаётся достичь желаемого результата. В этой связи представляют интерес факторы, влияющие на результаты лечения ДО у детей в разных периодах формирования прикуса.
Цель
Изучить результаты двухэтапного ортодонтического лечения у детей с зубоальвеолярной формой ДО на примере клинического случая.
Материал и методы исследования
Проведён подробный анализ материалов, отражающих результаты лечения ребёнка в динамике в возрасте от 6 до 17 лет, в их числе медицинская карта стоматологического больного, фотографии лица, диагностические модели челюстей, ортопантомограммы.
Предварительный диагноз формулировали на основании данных основных (клинических) методов исследования — опрос, осмотр, клинические функциональные пробы. При опросе уточняли вероятные причины возникновения ДО и жалобы пациента и его родителей. При осмотре изучали отклонения конфигурации лица от общепринятых критериев нормы, а также проявления зубочелюстных аномалий. Функциональная проба по Эшлеру–Биттнеру демонстрировала состояние профиля лица при сагиттальных перемещениях нижней челюсти в сравнении с критериями нормальной окклюзии по Энглю.
Для уточнения полученных сведений применяли дополнительные (инструментальные) методы: фотометрию лица, измерение диагностических моделей челюстей, ортопантомографию. На фотографиях лица в прямой проекции изучали симметричность, пропорциональность, определяли тип лица по Izard. В боковой проекции оценивали профиль, эстетичность лица по методу Ricketts. На диагностических моделях челюстей измеряли высоту и ширину коронок постоянных зубов в сравнении с нормой по В.Л. Устименко. Пропорциональность сегментов зубных рядов изучали по методам Tonn, Gerlach. Ширину, длину, симметричность зубных рядов оценивали с применением методов Pont, Korkhaus, Ф.Я. Хорошилкиной [1–3, 6, 20].
Методом ортопантомографии проводили оценку зубоальвеолярных областей, временных и постоянных зубов, костной ткани верхней и нижней челюстей, височно-нижнечелюстных суставов [22–24].
Проведённое исследование соответствует стандартам Хельсинкской декларации (Declaration Helsinki). В медицинской карте ортодонтического пациента (учётная форма №043-1/у), утверждённой приказом Минздрава России от 15.12.2014 №834н, есть информированное согласие на проведение ортодонтического лечения и использование обезличенных фотографий его зубов и полости рта («я разрешаю использовать фотографии моих зубов и полости рта без указания моих имени и фамилии»).
Результаты и обсуждение
Из медицинской карты следует, что за ортодонтической помощью пациент Л. впервые обратился в возрасте 5 лет с жалобами на неправильное положение нижних резцов, которое родители выявили в период их прорезывания.
Из анамнеза. Ребёнок родился в срок, доношенным, рос и развивался в соответствии с возрастом. Соматические заболевания на момент обращения не выявлены. Наследственный характер зубочелюстных аномалий не установлен. К стоматологу за лечением кариеса зубов не обращались, зуб 8.4 удалили по причине осложнённого кариеса в возрасте 6 лет.
Конфигурация лица пациента изменена незначительно. Однако были выявлены чрезмерный изгиб шейного отдела позвоночника и наклон головы назад, что рассматривали как фактор риска формирования нижней микро/ретрогнатии и ухудшения профиля лица [25].
При осмотре полости рта выявлено отсутствие в зубном ряду зуба 8.4, оценённое нами как фактор риска возникновения деформации с укорочением нижнего зубного ряда на стороне удаления [26–28].
Взаимоположение дистальных поверхностей коронок верхних и нижних вторых временных моляров в одной плоскости предполагало прорезывание первых постоянных моляров по II классу Энгля.
По результатам обследования был сформулирован диагноз: «Нейтральная окклюзия, сужение зубных рядов, тесное положение резцов. Вторичная адентия зуба 8.4».
Пациенту была рекомендована лечебная физкультура для нормализации осанки. Изготовлены съёмные пластиночные устройства, расширяющие зубные ряды. Восстановлен дефект нижнего зубного ряда справа для предупреждения нежелательной миграции зубов в сторону дефекта, сокращения бокового сегмента и нарушения контактов зубов-антагонистов.
Предложенные меры были предназначены для устранения имеющихся отклонений от нормы, профилактики отрицательного воздействия выявленных факторов риска и создания условий для формирования физиологической окклюзии. Однако пациент отказался пользоваться ортодонтическими устройствами и не посещал ортодонта в течение 1,5 лет.
В возрасте 8 лет пациент повторно обратился к ортодонту с жалобами на тесное положение нижних резцов. Сохранялись чрезмерный изгиб шейного отдела позвоночника и наклон головы назад. Уменьшение высоты нижней трети лица в сравнении с высотой средней трети лица на 2,0 мм сопровождалось незначительными изменениями конфигурации лица.
Лицевой морфологический индекс по Izar оказался равным 87,5%, что не противоречило сведениям о нарушении пропорциональности среднего и нижнего отделов лица и уменьшении высоты нижнего отдела лица (oph-sn) >(sn-gn). Пропорциональность отделов нижней трети лица была также нарушена (sn-st):(st-gn)=1:2,2.
На фотографиях лица в боковой проекции контуры губ и мягких тканей подбородка оставались в профильном поле Дрейфуса. Профиль лица выпуклый (угол n-sn-pg=164°). Выступающие точки губ не касались эстетической линии по Ricketts (pn-pg).
При осмотре полости рта выявили тесное положение нижних резцов, вторичную адентию зуба 8.4, укорочение правого бокового сегмента и асимметрию нижнего зубного ряда. Диастема между зубами 1.1 и 2.1 сочеталась с недостатком места в зубном ряду для прорезывания боковых резцов верхней челюсти. Средние линии зубных рядов не совпадали. Соотношение зубных рядов в области первых постоянных моляров справа и слева было по II классу, а в области временных клыков слева физиологическое, справа бугорковое, что, по нашему мнению, было следствием смещения зуба 8.3 в сторону дефекта нижнего зубного ряда.
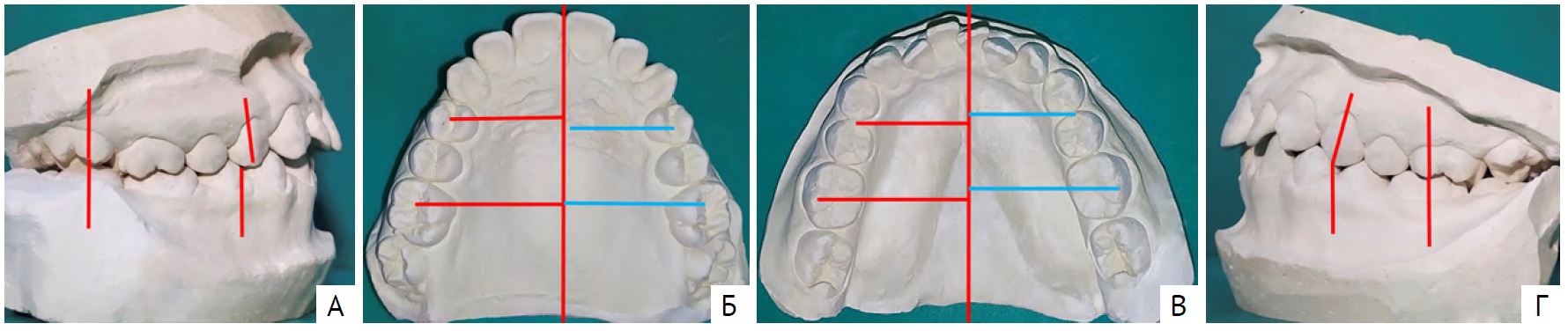
На диагностических моделях челюстей (рис. 1) изучали ширину и длину передних отделов зубных рядов по методам Pont и Korkhaus. По причине отсутствия в ряду зубов 1.2 и 2.2 сумму ширины коронок резцов верхней челюсти вычисляли по формуле с применением индекса Tonn (SI'=si×4/3). Выявили сужение зубных рядов, укорочение правого бокового сегмента и асимметрию нижнего зубного ряда.
Рис. 1. Диагностические модели челюстей пациента Л., возраст 8 лет 6 мес: А — вид справа; Б — модель верхней челюсти; В — модель нижней челюсти; Г — вид слева
На ортопантомограмме направление прорезывания зачатков постоянных зубов было нарушено, выявлен недостаток места в дуге для прорезывания боковых резцов (рис. 2).
Рис. 2. Ортопантомограмма пациента Л., возраст 8 лет 6 мес
Сформулировали диагноз: «ДО, зубоальвеолярная форма. Сужение зубных рядов. Асимметрия нижнего зубного ряда, укорочение бокового сегмента справа. Скученность и тортопозиция нижних резцов. Диастема в области зубов 1.1 и 2.1».
Сравнение формулировки диагноза с предыдущим указывало на ухудшение клинической ситуации, о чём пациент Л. и его родители были предупреждены. Обратили их внимание на наличие факторов риска формирования зубочелюстных аномалий: задержку прорезывания постоянных резцов, асимметрию нижнего зубного ряда, укорочение правого сегмента нижнего зубного ряда.
Составили план лечения: «Расширить зубные ряды при помощи съёмных пластиночных устройств механического действия, удлинить нижний зубной ряд справа. Осуществлять коррекцию направления прорезывания резцов и их положения в зубном ряду, контролировать соотношение первых постоянных моляров и временных клыков. Исключить функциональные нарушения и «вредные привычки».
Отсутствие нарушений гармоничности лица и имеющийся в этом возрасте потенциал роста пациента позволяли прогнозировать положительный результат лечения.
В возрасте 12 лет по причине задержки прорезывания постоянных зубов и неравномерной резорбции корней временных моляров [28] пациент был направлен на ортопантомографию и удаление временных зубов (рис. 3).
Рис. 3. Ортопантомограмма пациента Л. 12 лет
Составлен план лечения: «Расширить зубные ряды при помощи съёмных ортодонтических устройств с винтами и дистализировать первые постоянные моляры до их соотношения по I классу Энгля. Осуществлять контроль прорезывания клыков и премоляров. Исключить функциональные нарушения». Получен удовлетворительный результат лечения (рис. 4).
Рис. 4. Диагностические модели челюстей пациента Л. 13 лет: А — вид справа; Б — модель верхней челюсти; В — модель нижней челюсти; Г — вид слева
Достигнута нейтральная окклюзия. Устранено глубокое резцовое перекрытие. Положение резцов улучшилось, сохранялось тесное их положение. Создано место для прорезывания клыков и премоляров. Обращала на себя внимание задержка сроков прорезывания постоянных клыков, вторых премоляров и вторых моляров. Было рекомендовано исключить функциональные нарушения и «вредные привычки», посещать ортодонта 2 раза в год для контроля над формированием постоянного прикуса. Однако пациент не посещал ортодонта.
В возрасте 15 лет пациент вновь обратился к ортодонту с жалобами на тесное положение нижних резцов.
В результате занятий спортом улучшились осанка и наклон головы. Обращали на себя внимание напряжение мимических мышц лица и незначительное ограничение открывания рта. Конфигурация лица в покое была гармоничной, в момент окклюзии высота нижней трети лица была меньше нижней трети лица на 2,0 мм.
Выявили «вредную привычку» опираться рукой на подбородок. Родителям и пациенту разъясняли необходимость соблюдения правильной осанки, исключения «вредных привычек», функциональных нарушений [29]. На диагностических моделях челюстей (рис. 5) определили правильные фиссурно-бугорковые контакты боковых зубов. Перекрытие нижних резцов оказалось больше 1/2 высоты коронок сопровождалось их тесным положением и тортопозицией.
Рис. 5. Диагностические модели челюстей пациента Л. 15 лет: А — вид справа; Б — модель верхней челюсти; В — модель нижней челюсти; Г — вид слева
Измерение на диагностических моделях челюстей ширины и высоты коронок постоянных зубов показало, что параметры одноимённых зубов асимметричны. Ширина коронок отдельных зубов, в частности, зубов 1.7, 1.1, 2.1, 2.3, 2.7, 3.1, 4.1, превышала среднестатистическую норму (табл. 1).
Таблица 1. Ширина и высота коронок постоянных зубов и их отличия от индивидуальной нормы
Ширина и высота коронок зубов (норма по В.Л. Устименко) | ||||||||||||||
Ширина норма | 8,7–10 | 8,7–10 | 6,0–7,0 | 6,2–7,2 | 7,1–8,1 | 6,0–7,1 | 8,0–9,0 | 8,0–9,0 | 6,0–7,1 | 7,1–8,1 | 6,2–7,2 | 6,0–7,0 | 8,7–10 | 8,7–10 |
Ширина | 12,0 | 9,9 | 6,3 | 6,4 | 7,7 | 7,0 | 8,7 | 8,6 | 6,6 | 7,9 | 6,4 | 6,6 | 9,7 | 10,8 |
Высота норма | 4,5–5,9 | 4,5–5,9 | 5,3–6,9 | 6,6–8,0 | 8,0–9,6 | 7,1–8,5 | 8,2–9,7 | 8,2–9,7 | 7,1–8,5 | 8,0–9,6 | 6,6–8,0 | 5,3–6,9 | 4,5–5,9 | 4,5–5,9 |
Высота | 5,6 | 5,4 | 5,9 | 7,8 | 8,4 | 8,1 | 10,6 | 10,6 | 8,5 | 10,0 | 8,0 | 6,1 | 5,5 | 5,4 |
Зубы в/ч | 17 | 16 | 15 | 14 | 13 | 12 | 11 | 21 | 22 | 23 | 24 | 25 | 26 | 27 |
Зубы н/ч | 47 | 46 | 45 | 44 | 43 | 42 | 41 | 31 | 32 | 33 | 34 | 35 | 36 | 37 |
Высота | 5,1 | 5,2 | 6,2 | 7,4 | 8,5 | 8,3 | 9,0 | 8,8 | 8,3 | 8,7 | 7,8 | 6,4 | 6,0 | 5,9 |
Высота норма | 4,5–5,9 | 4,4–6,1 | 6,0–7,3 | 7,2–8,5 | 8,5–10,2 | 7,2–8,7 | 7,0–8,6 | 7,0–8,6 | 7,2–8,7 | 8,5–10,2 | 7,2–8,5 | 6,0–7,3 | 4,4–6,1 | 4,5–5,9 |
Ширина | 10,0 | 10,4 | 7,3 | 7,3 | 6,6 | 5,7 | 5,4 | 5,4 | 5,6 | 6,8 | 7,1 | 7,4 | 11,2 | 10,1 |
Ширина норма | 9,6–10,8 | 10,3–11,7 | 6,5–7,4 | 6,4–7,3 | 6,3–7,2 | 5,6–6,4 | 4,9–5,6 | 4,9–5,6 | 5,6–6,4 | 6,3–7,2 | 6,4–7,3 | 6,5–7,4 | 10,3–11,7 | 9,6–10,8 |
Примечание: в/ч — верхняя челюсть; н/ч — нижняя челюсть.
Отклонения ширины коронок отдельных зубов от среднестатистической нормы способствовали диспропорции сегментов зубных рядов.
Пропорциональность ширины коронок постоянных зубов и протяжённости сегментов зубных рядов по Tonn и Korkhaus представлены в табл. 2.
Таблица. 2. Сегментарный анализ зубных рядов
Сегментарный анализ зубных рядов по методу Gerlach в периоде постоянного прикуса | |||||||||
Lor | Lur | Lol | Lul | SI | si | ||||
сумма | измер. | сумма | измер. | сумма | измер. | сумма | измер. | ||
30,3 | 33,2 | 31,6 | 35,0 | 30,6 | 34,1 | 32,5 | 34,2 | 30,9 | 22,1 |
Примечание: измер. — измерение. Соотношение сегментов зубных рядов следующее: Si/si=1,398; Lor <Lur на 1,3 мм; Lor <Lur на 1,9 мм.
Ортодонтическая помощь в периоде сменного прикуса позволила расширить нижний зубной ряд и устранить его асимметрию, тем самым уменьшить скученность резцов и обеспечить условия для прорезывания клыков и премоляров. В результате многолетней реабилитации деформации зубных рядов у пациента были максимально устранены, однако получить «идеальный» результат не удалось (рис. 6).
Рис. 6. Cегментарный анализ по методу Gerlach зубных рядов верхней (А–Г) и нижней (Д–З) челюстей пациента Л. в возрасте от 8 лет 6 мес до 17 лет
Отклонения ширины коронок зубов от нормы, нарушения пропорциональности сегментов зубных рядов затрудняли формирование окклюзии в соответствии с «шестью ключами» по Эндрюсу.
Кроме того, на ортопантомограмме выявили искривление корней постоянных зубов (рис. 7), что затрудняло их перемещение, а нормализация наклона корней при этом не представлялась возможной.
Рис. 7. Ортопантомограмма пациента Л. 15 лет
Пациент и родители были предупреждены о вероятности возникновения некоторых проблем при перемещении зубов и формировании окклюзии. С планом лечения пациент и его родители согласились. Однако обратились с просьбой удалить зачатки третьих моляров позже, мотивируя семейными обстоятельствами.
В результате ортодонтического лечения брекет-системой Damon Q с соответствующими силовыми элементами получен удовлетворительный результат (рис. 8).
Рис. 8. Диагностические модели челюстей пациента Л. 17 лет: А — вид справа; Б — модель верхней челюсти; В — модель нижней челюсти; Г — вид слева
На ортопантомограмме после завершения ортодонтической коррекции окклюзии выявлены незначительная асимметрия положения зубов и искривление корней отдельных зубов (рис. 9).
Рис. 9. Ортопантомограмма пациента Л. 17 лет
Положение зачатков зубов 2.8, 3.8 и 4.8 в динамике наблюдения от 15 до 17 лет ухудшилось (рис. 10).
Рис. 10. Изменение наклона нижних третьих постоянных моляров пациента Л. относительно окклюзионной плоскости на ортопантомограммах в возрасте 15–17 лет
Это подтверждала динамика наклона осей постоянных зубов и зачатков третьих постоянных моляров относительно окклюзионной плоскости (табл. 3).
Таблица 3. Наклон осей постоянных зубов пациента Л. в динамике наблюдения методом ортопантомографии
Возраст | Наклоны осей в градусах постоянных зубов верхней челюсти | |||||||||||||||
18 | 17 | 16 | 15 | 14 | 13 | 12 | 11 | 21 | 22 | 23 | 24 | 25 | 26 | 27 | 28 | |
8,5 лет | 47,4 | 63,1 | 66,6 | 105 | 93 | 85 | 85 | 96 | 101,9 | 93 | 78,8 | 108,9 | 119,2 | 140,9 | ||
12,5 лет | 77,7 | 75 | 90,7 | 91,6 | 90,6 | 77,3 | 93,6 | 93,3 | 108,8 | 86,8 | 92,2 | 98,4 | 110 | 117,8 | ||
15 лет | 65 | 84,9 | 91,2 | 86,7 | 85,5 | 82,8 | 92,2 | 88,5 | 99 | 86,8 | 87,4 | 93,1 | 100,5 | 121,4 | 132,7 | |
17 лет | 70,9 | 71,3 | 82,9 | 85,7 | 86,3 | 81,9 | 87,1 | 87,7 | 101,4 | 91,8 | 87,7 | 97,7 | 97,2 | 113 | 155 | |
Возраст | Наклоны осей в градусах постоянных зубов нижней челюсти | |||||||||||||||
48 | 47 | 46 | 45 | 44 | 43 | 42 | 41 | 31 | 32 | 33 | 34 | 35 | 36 | 37 | 38 | |
8,5 лет | 123,4 | 120,6 | 105,3 | 100,2 | 117,3 | 92 | 91 | 98,7 | 95,8 | 58,2 | 83,7 | 84,8 | 64,3 | 53,5 | ||
12 лет | 115,5 | 111,5 | 103,5 | 93,8 | 96,6 | 91,6 | 91,6 | 93,1 | 98,3 | 89,3 | 81,4 | 81,4 | 66,3 | 62,6 | ||
15 лет | 132,4 | 100,2 | 104,3 | 102 | 96,6 | 94,3 | 89,4 | 87,8 | 85,4 | 92,7 | 83,7 | 85,8 | 78,8 | 74,2 | 81,4 | 130,8 |
17 лет | 141,4 | 112,8 | 111,6 | 113,6 | 97,1 | 104,3 | 83,3 | 90,9 | 85,5 | 86,3 | 77 | 80 | 76,2 | 111,5 | 64,2 | 140,8 |
Таким образом, результаты нашего исследования показали ряд факторов, оказавших влияние на развитие зубочелюстных аномалий и эффективность лечения у пациента с ДО.
Несвоевременное обращение за специализированной стоматологической помощью и преждевременная потеря временного моляра привели к асимметрии нижнего зубного ряда и увеличению тяжести зубочелюстных аномалий.
Недостаточной оказалась мотивация [30] к устранению «вредных привычек». Регулярная опора подбородком на ладонь руки способствовала увеличению степени перекрытия резцов.
Несоблюдение рекомендаций по улучшению осанки и сохранение чрезмерного изгиба шейного отдела позвоночника и наклона головы назад также отразились на формировании окклюзии.
Несвоевременное удаление зачатков третьих постоянных моляров [31] и нарушения развития отдельных постоянных зубов препятствовали полноценной коррекции положения зубов при помощи эффективной современной несъёмной ортодонтической техники (брекет-системы Damon Q).
Выводы
- Конфигурация лица в сагиттальном направлении при зубоальвеолярной форме дистальной окклюзии гармоничная. При сочетании дистальной окклюзии с глубокой резцовой окклюзией возможно уменьшение высоты нижнего отдела лица.
- Преждевременная потеря временного моляра (зуба 8.4), нарушение развития отдельных зубов и задержка их прорезывания, функциональные нарушения и «вредные привычки» способствовали возникновению деформаций нижней зубной дуги, повышению тяжести зубочелюстных аномалий и снижению эффективности вторичной профилактики и ортодонтического лечения пациента с зубоальвеолярной формой дистальной окклюзии.
- Преждевременная потеря временного моляра с одной стороны привела к сокращению протяжённости бокового сегмента и асимметрии зубоальвеолярной дуги, нарушению окклюзионных контактов. Устранение этих деформаций вызвало необходимость применения дополнительных ортодонтических устройств.
- Задержка смены временных зубов предположительно может стать причиной искривления корней прорезывающихся постоянных зубов, является показанием к удалению этих временных зубов.
- Асимметрия размеров коронок зубов и искривление корней отдельных постоянных зубов затрудняли достижение ортодонтического результата в соответствии с общепринятыми «шестью ключами окклюзии» по Эндрюсу.
- На формирование зубочелюстных аномалий и результаты ортодонтического лечения оказали влияние недостаточная мотивация к активному сотрудничеству пациента и его близких со специалистами стоматологического профиля.
- Аномальное направление прорезывания зачатков третьих моляров сохранялось в динамике наблюдения в периоде сформированного постоянного прикуса.
Участие авторов. Ф.С.А. — руководство работой, анализ литературных сведений и результатов исследования; Р.А.Х. — проведение исследования, анализ литературных сведений и результатов исследования.
Источник финансирования. Исследование не имело спонсорской поддержки.
Конфликт интересов. Авторы заявляют об отсутствии конфликта интересов по представленной статье.
About the authors
Farida S Ayupova
Kuban State Medical University
Author for correspondence.
Email: farida.sag@mail.ru
ORCID iD: 0000-0002-4194-664X
SPIN-code: 5187-5443
Scopus Author ID: 57193081297
ResearcherId: AAM-4413-2021
MD, Cand.Sci. (Med.), Assoc. Prof., Depart. of Pediatric Dentistry, Orthodontics and Oral Surgery
Russian Federation, Krasnodar, RussiaRasudan A Khotko
Kuban State Medical University
Email: khotko.rasudana@yandex.ru
ORCID iD: 0000-0003-0711-0838
SPIN-code: 3593-1187
ResearcherId: AAJ-64362021
MD, Resident, Depart. of Stomatology, faculty of advanced training and professional retraining of specialists
Russian Federation, Krasnodar, RussiaReferences
- Khoroshilkina FYa. Rukovodstvo po ortodontii. (A guide in orthodontics.) 2nd ed. Мoscow: Medicine; 1999. 800 p. (In Russ.)
- Khoroshilkina FYa. Orthodontia. (Orthodontics.) 2nd ed. Мoscow: MIA; 2010. 592 p. (In Russ.)
- Persin LS. Ortodontiya. Natsional'noe rukovodstvo. Vol. 1. Diagnostika zubochelyustnykh anomaliy. (Orthodontics. National guide. In 2 vol. Vol. 1. The diagnostics of the dentoalveolar abnormalities.) Ed. by LS Persin. Moscow: GEOTAR-Media; 2020. 304 p. (In Russ.) doi: 10.33029/9704-5408-4-1-ONRD-2020-1-304.
- Ayupova FS, Voskanyan AR. Structure of dental alveolar anomalies in children in the regions of Russia and in the near and far abroad (literature review). Pediatric dentistry and dental prophylaxis. 2016;(3):49–55. (In Russ.)
- Ayupova FS, Tereshchenko LF. Structure of dental alveolar anomalies in children taking orthodontic advice. Kursk Scientific and Practical Bulletin “Man and His Health”. 2013;(4):50–54. (In Russ.)
- Obrazcov YuL, Larionov SN. Propedevticheskaya ortodontiya. (Propaedeutic orthodontics.) Saint-Petersburg: SpecLit; 2007. 210 p. (In Russ.)
- Mitchell L. An introduction to orthodontics. Oxford (UK): Oxford University Press; 2013. 228 p. Russ ed.: Mitchell L. Osnovy ortodontii. Ed. by Yu.M. Malygin. Moscow: GEOTAR-Media; 2017. 336 p. (In Russ.)
- Espeland LV, Stenvik A. Perception of personal dental appearance in young adults: relationship between occlusion, awareness, and satisfaction. Am J Orthod Dentofacial Orthop. 2008;100(3):234–241. doi: 10.1016/0889-5406(91)70060-A.
- Proffit WR. Contemporary orthodontics. 5th ed. St. Louis, Mo.: Elsevier/Mosby, 754 p. Russ ed.: Proffit WR. Sovremennaya ortodontiya. Moscow: MEDpress-inform; 2019. 712 p.
- Persin LS. Ortodontiya. Natsional'noe rukovodstvo. T. 2. Lechenie zubochelyustnykh anomaliy. (Orthodontics. National guide. Vol. 2. The treatment of the dentoalveolar abnormalities.) Ed. by LS Persin. Moscow: GEOTAR-Media; 2020. 376 p. (In Russ.) doi: 10.33029/9704-5409-1-2-ONRD-2020-1-376.
- Persin LS, Sharov MN. Stomatologiya. Neyrostomatologiya. Disfunktsii zubochelyustnoy sistemy. (Dentistry. Neurostomatology. Dysfunctions of the dentoalveolar system.) Moscow: GEOTAR-Media; 2013. 360 p. (In Russ.)
- Ayupova FS, Khotko RA. Modern trends in the choice of tactic and method for the treatment of growing patients with distal occlusion (literature review). Pediatric dentistry and dental prophylaxis. 2020;20(2):156–159. (In Russ.) doi: 10.33925/1683-3031-2020-20-2-156-159.
- Malygin YuM, Pyleva NV. Evaluation of different orthodontic facilities effectiveness while distal placement of lateral teeth. Clinical dentistry. 2009;(3):64–67. (In Russ.)
- Karton EA. Organizing and planning comprehensive rehabilitation programs for patients with sagittal abnormalities of occlusion. Social aspects of public health. 2015;(3):8. (In Russ.)
- Veretennikova OP, Gvozdeva LM. Integrated approach in the treatment of children with distal malocclusion during early mixed dentition. Dental Forum. 2014;(4):38–42. (In Russ.)
- Doroshenko SI, Kulginskiy EA, Storozhenko KV. Specificities of orthodontic treatment of patients with distal occlusion in different age periods of the dentoalveolar system’s formation. Modern orthodontics. 2012;(3):5–12. (In Russ.)
- Graber TM, Vanarsdall RLJr. Orthodontics. Current principles and techniques. Book. 5th ed. Mosby; 2011. 994 p.
- Patti A, Perrier G. Clinical success in early orthodontic treatment. Quintessence International; 2005. 124 p.
- Malnagren О, Omblus J, Hagg U, Pancherz H. Treatment with an orthopedic appliance system in relation to treatment intensity and growth periods. A study of initial effects. Am J Orthod Dentofac Orthop. 1987;191:143–151. doi: 10.1016/0889-5406(87)90472-0.
- Nabatchikova LP, Horoshilkina FYa, Chobanyan Arman, Chobanyan Armine. Differences in the sizes of crowns of primary molars and premolars and their significance for the choice of preventive measures at the sagittal occlusion dentition anomalies. IP Pavlov Russian Medical Biological Herald. 2014;(3):132–138. (In Russ.)
- Khoroshilkina FYa, Frenkel R, Demner LM, Falk F, Malygin YuM. Diagnostika i funktsional'noe lechenie zubochelyustno-litsevykh anomaliy. (Diagnosis and functional treatment of maxillofacial anomalies.) Мoscow: Medicine; 1987. 304 p. (In Russ.)
- Vasilyev AY. Luchevaya diagnostika v stomatologii. Natsional'noe rukovodstvo. (Radiodiagnostics in dentistry. National guide.) Ed. by A.Y. Vasilyev, S.K. Ternovoy. Moscow: GEOTAR-Media; 2010. 288 p. (In Russ.)
- Morozova NV, Vasmanova EV, Landinova VD, Golochalova NV, Ivankina EO. Possibility of radiologic research in children preventive dentistry. Stomatologiya detskogo vozrasta i profilaktika. 2014;13(3):3–7. (In Russ.)
- Ayupova FS, Pavlyi YuS. Opportunities of orthopantomography for children with dentoalveolar anomalies. Pediatric dentistry and dental prophylaxis. 2016;(1):34–38. (In Russ.)
- Zvolinska AM, Mozoliuk EYu. Teenagers’ and childrens’ postural disorder as a cause for wrong occlusion development. Sovremennaya stomatologiya. 2018;(1):90. (In Ukr.)
- Morozova NV, Slabkovskaya AB. Effect of premature loss of primary teeth on permanent teeth development. Ortodontiya. 2016;(4):2–7. (In Russ.)
- Yakhina ZKh, Shiryak TY, Kamaldinova AR. Effect of early loss of teeth on formation of dental anomalies. Modern Problems of Science and Education. 2018;(2):57. (In Russ.)
- Ayupova FS, Alekseenko SN, Zobenko VYa, Gayvoronskaya TV. Resorption of multirooted temporary teeth in children with dentofacial anomalies in accordance with the orthopantomography data. Pediatric dentistry and dental profilaxis. 2020;20(3):235–241. (In Russ.) doi: 10.33925/1683-3031-2020-20-3-235-241.
- Ushnitskiy ID, Alexeeva ТV, Pinelis IS, Yurkevich АV, Mikhalchenko DV, Davidov IЕ. Etiologic factors and pathogenic mechanisms of dent-alveolar deformities formation and development. Dal'nevostochnyy meditsinskiy zhurnal. (In Russ.) doi: 10.35177/1994-5191-2019-2-93-98.
- Zinchenko KS, Dudukalova VS, Khachatryan AZ, Sadovnikova TG, Voloshina OV. Orthodontic treatment motivation and cooperation: analysis of adolescent patients’ and parents’ responses. Meditsina. Sotsiologiya. Filosofiya. Prikladnye issledovaniya. 2020;(3):7–11. (In Russ.)
- Arsenina OI, Shishkin KM, Shishkin MK, Popova NV. The third permanent molars and their influence on the dentoalveolar arches. Russian journal of stomatology. 2016;2(9):33–40. (In Russ.) doi: 10.17116/rosstomat20169233-40.
Supplementary files